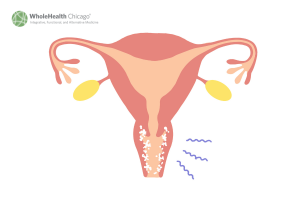
In our recent Health Tip, we delved into the intricate world of Candida and yeast infections, but when it comes to sheer prevalence, the most common vaginal ailment is Bacterial Vaginosis (B.V., for brevity), typically ignited by a variety of culprits, with Gardnerella being the prime suspect. While B.V. isn’t classified as a traditional sexually transmitted disease (STD), it predominantly affects sexually active women. This condition arises due to shifts in vaginal conditions, triggered by factors such as antibiotics, changes in birth control methods, well-meaning douching practices, and even wardrobe choices like spandex or nylon underwear. Symptoms vary from absence (detected incidentally during routine PAP smears) to a thin, greyish-white, and itchy discharge. A savvy health care practitioner can diagnose B.V. based on symptoms, discharge appearance, and microscopic examination. The standard prescription often includes metronidazole, available as a vaginal cream or tablet, but boric acid suppositories have also been a trusted option for nearly a century. Additionally, maintaining a healthy vaginal microbiome with probiotics can be beneficial.
Tag: joint pain
Common Vaginal Infections, Number 1: CANDIDA
In the realm of women’s health, few topics carry as much importance and intrigue as common vaginal infections, and Candida, often synonymous with “yeast infections,” holds a prominent place in this narrative. Candida, those resilient single-cell organisms, have coexisted with us since time immemorial, occasionally venturing into the spotlight when things down there fall out of balance. This blog post delves into the world of Candida, discussing its prevalence, symptoms, and factors that can tip the scales in its favor. From the relentless use of antibiotics to the sweet tooth of diabetics, we explore the intricate dynamics of Candida overgrowth and offer insights into managing these troublesome vaginal infections. So, join us on this journey into the realm of women’s health as we unravel the Candida conundrum and empower you with knowledge to foster a healthier vaginal microbiome.
Peptide Therapy: Thymosin and BPC-157
Honestly, if you Google ‘peptide therapy’, you’ll get overwhelmed by TMI (‘too much information’). Then you might be put off by claims that sound terrific (“Burn fat! Combat mental decline!” “Heal wounds! Reverse aging!”) but then make you feel, well, skeptical. Let’s face it, we’d all like ‘enhanced fat burning,’ ‘better wound healing’, ‘smoother skin’, […]
Orthomolecular Medicine and Longevity
“Orthomolecular medicine”. Now there’s a phrase you don’t hear in the 21st century, except in historical terms. Invented by two-time Nobel Prize winner Dr. Linus Pauling (Do you even remember him? Ah! How fleeting is fame!), one prize for his work on chemical bonds, the second, the Nobel Peace Prize for his work banning atmospheric […]
Everything Begins In The Gut
I sometimes wonder if new patients to WholeHealth Chicago think we’re overly preoccupied with their digestion, gut health, nutrition, and even the consistency and quality of their stool when they scheduled that appointment for a seemingly unrelated problem. We certainly treat a large variety of health concerns: anti-aging and disease prevention, dermatologic problems, chronic fatigue, […]
Lyme: The Latest
I’d guess that Lyme disease nears the top of the “more info please” requests I receive from both Health Tip readers and WholeHealth Chicago patients. There are three good reasons for this concern: Lyme disease is definitely on the upswing, both actual patient numbers and geographic spread. Treatment, especially for chronic Lyme, can be a […]
Flu
Although medical textbooks list hundreds of different illnesses, a bad case of flu is high on the list of those that make you feel the sickest. Those who have really had the “flu” (and I’m not talking about a bad cold, although a mild case of the flu is indistinguishable from a bad cold) will know exactly what I’m talking about. It seems that your every muscle aches; you feel so weak you can barely click the remote on your TV; your mind is so foggy that comic books are challenging; and your throat is raw from a cough that brings up no phlegm. Conventional medicine can offer some help: If you’re at a high risk for flu, vaccines can reduce your risk of getting flu during an epidemic; antiviral medications can help (somewhat) check the spread of the germ to other members of your family; antibiotics can help you deal with bacterial superinfection, if you develop one.