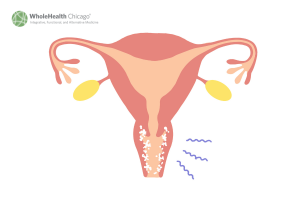
In our recent Health Tip, we delved into the intricate world of Candida and yeast infections, but when it comes to sheer prevalence, the most common vaginal ailment is Bacterial Vaginosis (B.V., for brevity), typically ignited by a variety of culprits, with Gardnerella being the prime suspect. While B.V. isn’t classified as a traditional sexually transmitted disease (STD), it predominantly affects sexually active women. This condition arises due to shifts in vaginal conditions, triggered by factors such as antibiotics, changes in birth control methods, well-meaning douching practices, and even wardrobe choices like spandex or nylon underwear. Symptoms vary from absence (detected incidentally during routine PAP smears) to a thin, greyish-white, and itchy discharge. A savvy health care practitioner can diagnose B.V. based on symptoms, discharge appearance, and microscopic examination. The standard prescription often includes metronidazole, available as a vaginal cream or tablet, but boric acid suppositories have also been a trusted option for nearly a century. Additionally, maintaining a healthy vaginal microbiome with probiotics can be beneficial.
Tag: antibiotics
Common Vaginal Infections, Number 1: CANDIDA
In the realm of women’s health, few topics carry as much importance and intrigue as common vaginal infections, and Candida, often synonymous with “yeast infections,” holds a prominent place in this narrative. Candida, those resilient single-cell organisms, have coexisted with us since time immemorial, occasionally venturing into the spotlight when things down there fall out of balance. This blog post delves into the world of Candida, discussing its prevalence, symptoms, and factors that can tip the scales in its favor. From the relentless use of antibiotics to the sweet tooth of diabetics, we explore the intricate dynamics of Candida overgrowth and offer insights into managing these troublesome vaginal infections. So, join us on this journey into the realm of women’s health as we unravel the Candida conundrum and empower you with knowledge to foster a healthier vaginal microbiome.
Getting Tough With Your Immune System
No reasonable physician (I modestly include myself here) can refrain from crowing delightedly when a new clinical study confirms the value of a treatment he or she had been using for years, even if that treatment had contradicted prevailing standards. Ever since I learned something about natural medicine, I’ve been reluctant to prescribe antibiotics for […]
Getting Off Antidepressants (Or Avoiding Them Altogether)
There’s an uncanny similarity between antibiotic and antidepressant prescribing in the US. If you’re currently taking one or both, took them in the past, or are considering taking one or both now, know that the odds are very strong you don’t need either of them. Numerous clinical studies confirm that both antibiotics and antidepressants are […]
Six Commonly Missed Diagnoses: Candida (Yeast)
Posted 06/18/2012 Back in 1993, several weeks before the opening of what would be known as WholeHealth Chicago, I was summoned to the office of the chief of medicine at the hospital where I was a staff member. The chief had heard rumors I was opening a center that would combine conventional and alternative practitioners […]
Antibiotics: Maximize Benefits, Minimize Intestinal Backlash
Posted 02/20/2012 Patients seem to be divided equally in their attitude toward antibiotics. Either they love ‘em, remembering relief from a painful bladder infection, a nagging cough, or clogged sinuses, or they hate ‘em, recalling minimal relief along with lots of diarrhea and/or an industrial-strength vaginal yeast infection. That first group often progresses to what […]
Poisoned by an Antibiotic
Although he was only in his early thirties, he moved like an old man with widespread arthritis. At the stairs, he supported himself on the short banister to keep his full weight off his feet. It looked as if every one of his muscles were in pain.